Rectal Prolapse
Definition and Introduction
|
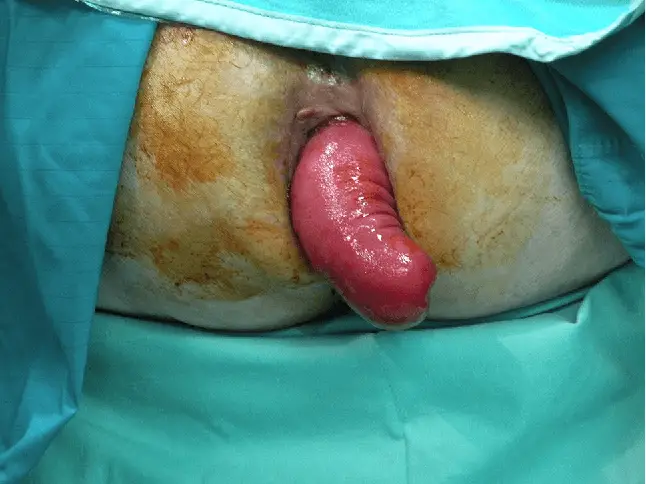
| Image courtesy of Semantic Scholar Opens in new window Rectal prolapse is a circumferential, full-thickness protrusion of the rectal wall through the anal orifice. It is often associated with other anatomical findings such as a redundant sigmoid colon, deep pelvic cul-de-sac (pouch of Douglas), and pelvic laxity. |
Rectal prolapse is commonly found in females with a female-to-male ratio that approaches 6:1 in adults. While the incidence of rectal prolapsed increases with increasing age in females, males have an equal incidence per decade through-out adult life. Women with rectal prolapsed also have a higher incidence of other associated pelvic disorders including urinary incontinence, rectocele, cystocele, and enterocele.
Pelvic floor disorders are a challenging and poorly understood clinical entity. These disorders are most commonly found among the elderly. Bharucha et al. demonstrated in a study known as the Women’s Health Initiative that nearly 40% of women 40 years or older suffer from defecatory dysfunction. In fact, 1 out of 10 women by the age of 80 will require surgery for pelvic organ prolapsed.
In a recent study of patients with pelvic floor disorders, rectal prolapse was found more commonly in those patient older than 70 than those younger than 70 (17 vs. 27%, respectivel). Less common associated conditions include connective tissue disorders such as Ehlers-Danlos syndrome, congenital hypothyroidism, and solitary rectal ulcer.
Rectal prolapse consists in three types:
- full-thickness rectal prolapse (procidentia),
- mucosal prolapse, and
- internal intussusception.
The current theory of why rectal prolapse occurs relates to disorders of defecation that lead to excessive straining. Overtime, this will weaken the supportive structures of the pelvic floor and sphincter complex allowing for herniation of bowel, bladder, or uterus through the pelvic outlet.
This weakening may be accelerated as a result of pelvic floor nerve injuries associated with vaginal birth. Longitudinal radiographic studies have demonstrated that the development of prolapse may be a gradual process which begins as internal rectal intussusception and progresses to frank prolapse.
Presentation and Associated Findings
In most instances, patients present after the rectum is noted by a practitioner or the patient to protrude abnormally from the anus. The rectum may spontaneously reduce or require manual reduction.
On rare occasions, the rectum may incarcerate requiring a laparotomy to reduce it to its normal location. It is important to differentiate full-thickness prolapse from mucosal prolapse which is 4th degree hemorrhoids. The classic distinction between full-thickness rectal prolapse and mucosal prolapse is the presence on physical exam of circumferential folds seen in full-thickness rectal prolapse and radial folds with mucosal prolapse. Internal prolapse is best seen on imaging studies and is often hard to fully appreciate on physical examination since the rectum does not protrude through the anus.
The symptoms commonly found with all types of rectal prolapse include:
- tenesmus,
- rectal bleeding,
- a palpable mass, and
- fecal soiling.
There are several functional pelvic floor disorders associated with rectal prolapse. The most common functional disorders are fecal incontinence Opens in new window and constipation Opens in new window.
There is an increased incidence of rectal prolapse among individuals with colonic inertia and obstructed defecation secondary to non-relaxing puborectalis. Defecation occurs through a coordinated effort involving relaxation of the anal sphincter complex as well as the puborectalis muscle.
The puborectalis muscle acts like a sling to create an angle between the rectum and the anal canal. Relaxation of this sling obliterates the angle providing a direct passage of stool from the rectum through the anal canal. Paradoxical puborectalis muscle contraction during defecation maintains or exaggerates the anorectal angle resulting in a functional resistance to defecation.
Fecal incontinence Opens in new window occurs in the majority of patients with all types of rectal prolapse and the incidence increases with increasing age and duration of the prolapse. It is thought that fecal incontinence is the result of a combination of an increase in intra-rectal pressure as a result of the prolapse.
The increase in the intra-rectal pressure minimizes the normal pressure difference which exists between the rectum and the anal canal resulting in incontinence. Stretch injury to the pudendal nerves may also accelerate symptoms of incontinence. The pudendal nerves innervate the anal sphincter complex and can be injured over time as a result of excessive straining and recurrent herniation of the pelvic floor.
Evaluation
All patients presenting with rectal prolapse should undergo a complete history and physical exam. Associated symptoms such as urinary incontinence Opens in new window, vaginal vault prolapse, fecal incontinence Opens in new window, and constipation Opens in new window should be ascertained.
Careful assessment of risk factors for anesthesia and the functional status of the patient should be performed because this information may affect the surgeon’s choice of procedure. The physical exam should include careful evaluation of the perineum and prolapsed rectum.
With the patient in lithotomy position, the perineum should be inspected in the relaxed position as well as during straining. During straining, the prolapsed rectum can often be seen. If a laxity exists within the rectovaginal septum, a rectocele may be present. A digital rectal exam performed during straining can often demonstrate the lack of fixation of the rectum as well as the presence of internal intussusception. If the prolapse is not easily demonstrated, the use of an enema may help.
Additional investigations in patients with rectal prolapse should include a colonoscopy or barium enema. Both tests provide an evaluation of the colonic mucosa for a lead point causing intussusception or other abnormalities such as diverticular disease or solitary rectal ulcer which may influence the type of procedure performed.
Since these patients can manifest with several associated pelvic floor abnormalities, an assessment of pelvic floor anatomy and physiology is required. Depending on associated symptoms, tests may include cinedefecography, pelvic floor dynamic magnetic resonance imaging (MRI), anorectal manometry, endorecal ultrasound, electromyography (EMG), and colon transit studies.
Cinedefecography and dynamic pelvic floor MRI are both useful tests in the evaluation of rectal prolapse. Importantly, these tests can identify associated pelvic floor abnormalities which occur comely with rectal prolapse.
Cinedefecography is a test performed by the instillation of contrast into the rectum, vagina, and bladder and allowing the patient to evacuate the contents in the normal sitting position while real time images are obtained.
Cinedefecography can detect occult intussusception and rectal prolapse with a sensitivity of 100% and a specificity of 93%. Other abnormalities that may be detected include paradoxical puborectalis contraction and pelvic floor weakness such as rectocele, enterocele, and cystocele. In contrast, dynamic pelvic floor MR is performed with the installation of contrast into the rectum and vagina, however, the patient must be kept in the supine position. The patient is asked to bear down to the point of defecation while images are obtained. This test will identify a pelvic floor hernia.
Anorectal manometry and endorectal ultrasound is performed when symptoms of fecal incontinence or obstructed defecation are identified alone with internal or external rectal prolapse. Patients with lower resting and maximum squeeze pressures are less likely to recover sphincter control following rectal prolapse repair. However, it is important to note that increasing age is associated with lower anal resting pressure, higher rectal pressure and rectal gradient during simulated evacuation, and a shorter balloon expulsion time in asymptomatic individuals.
The balloon expulsion test can be performed at the same time anorectal manometry is performed. The balloon catheter used during this procedure is inflated with 50–100 cc of water and the patient is asked to expel the balloon.
Patients without obstructed defecation should easily expel the balloon, whereas patients experiencing obstructed defecation cannot expel the balloon. Endorectal ultrasound may be useful for evaluation of occult sphincter defects especially in older parous women.
Colonic transit studies such as colonic scintigraphy and Sitzmark studies may be necessary in patients with long standing constipation who have rectal prolapse. Scintgraphy utilizes nuclear medicine principles. This study utilizes 24 radiopaque markers which are ingested by the patient.
Sequential daily plain abdominal films are performed to demonstrate the movement of stool throughout the colon. Patients with total colonic inertia will retain at least 80% of the markers equally distributed throughout the colon at 5 days. Patients with obstructed defecation will have markers concentrated near the rectosigmoid junction. Failure to recognize and treat a dysfunctional colon or obstructed defecation may result in continued straining and ultimately, recurrent prolapse.
Management Options
The goal of treatment is the restoration of normal anatomy and correction of any associated physiologic disorder. Successful treatment results in long-lasting symptom relief and is accomplished best by non-operative and operative techniques.
- Non-operative Management
Non-operative therapy should be initiated in all patients with disorders of defecation. Initial treatment should include dietary and lifestyle changes. A review of medications and dietary history will often guide this therapy.
It is well known that a high fiber therapy with a total of 40 g of fiber should be consumed daily. Furthermore, patients are instructed to consume more liquids that are not caffeinated. Daily exercise 20 min a day is not only healthy for the cardiovascular system but also healthy for the gastrointestinal system.
Biofeedback is the mainstay therapy for obstructed defecation secondary to paradoxical puborectalis contraction and internal intussusception. Biofeedback training is aimed at suppressing the inappropriate contraction of the pelvic floor during defecation. This may result in a reduction in the time spent straining at defecation and prevent recurrence of prolapse.
- Operative Management
Operative repair is indicated for full-thickness prolapse and mucosal prolapse. There is limited role for operative repair for internal intussusception and obstructed defecation. Several types of repairs for rectal prolapse exist and the indication for each type as well as the recurrence rate is listed in Table X.
| Procedure | Indication | Recurrence (%) |
|---|---|---|
| Anal encirclement | Low functional status, high surgical risk | 0–60 |
| Delorme | Low functional status, high surgical risk | 5–21 |
| Perineal rectosigmoidectomy | High surgical risk | 0–44 |
| Ripstein rectopexy (mesh) | Prolapse without constipation | 0–13 |
| Wells rectopexy (mesh) | Prolapse without constipation | 2–10 |
| Suture rectopexy | Prolapse without constipation | 0–5 |
| Resection rectopexy | Prolapse WITH constipation, no fecal incontinence | 0–6 |
| Anterior resection | Prolapse associated with severe solitary rectal ulcer syndrome | 4–9 |
| Ventral rectopexy (mesh) | Internal or external prolapse with constipation or fecal incontinence | 4–14 |
| Table X | Indications and recurrence rates for perineal vs. abdominal vs. abdominal procedures for full- procedures for full-thickness rectal prolapse | ||
Reported outcomes following repair include recurrence of prolapse and persistent or new symptoms of constipation or fecal incontinence. In general, the literature supports the use of abdominal procedures rather than perineal procedures for rectal prolapse because of the associated decrease in recurrence rates.
The goal of the abdominal approach, whether laparoscopic or open is mobilization and fixation of the anterior or posterior rectum to the presacral fascia. The goal of the perineal procedure is partial or complete removal of the prolapsed rectum through the perineum with minimal operative risk to the patient. Therefore, if a patient’s physical condition does not allow for an abdominal procedure, then a perineal procedure is warranted. However, with the advances in anesthetic techniques, nowadays, the physical state of the patient should drive the operative approach. Perineal approaches in active patients are more prone to failure.
See also:
- Adapted from: Pelvic Floor Dysfunction and Pelvic Surgery in the Elderly: An Integrated ... Authored By David A. Gordon, Mark R. Katlic
